Between every bone in the human body, there is a joint — and they’re immensely important. Without them, our bones would grind each other down, making movement impossible.
The spine is a prime example. Typically, every adult has 24 vertebrae, and each is separated with an intervertebral disc. Think of that disc as a shock-absorbing jelly donut; however, with age, those discs can give way to stress and bulge outward. Eventually, they can burst, causing inflammation and pain from pressure on the nerves.
This is referred to as a herniated disc, a very common condition that’s easily treatable.
So, what should you do if you think you have one? Let’s discuss more about herniated discs, how they can affect anyone, how to detect them, and what non-surgical treatments are available to you.
What is a Herniated or Bulging Disc?
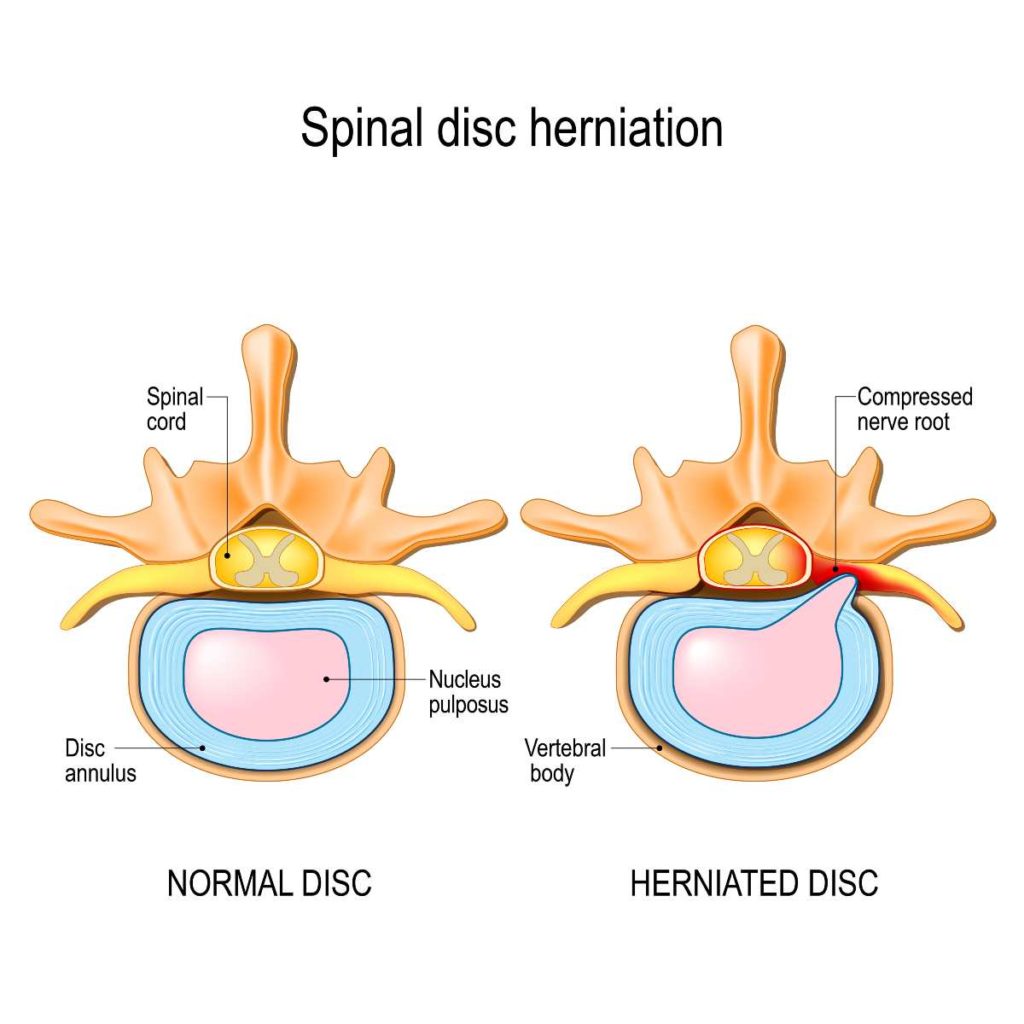
First, let’s explain what a disc is. Your spinal bones are separated by soft, elastic tissues called intervertebral discs — and yes, they’re very similar to that aforementioned jelly donut. The disc is called the nucleus pulposus, and it contains a soft and squishy interior made up of mostly water. The outside, or the annulus fibrosus, consists of fibrous collagen that’s tightly laced together to provide lots of flexibility.
A herniated disc — sometimes called a bulging or slipped disc — occurs when a disc or discs begin to bulge due to pressure. Eventually, they tear through the fibrous tissue; i.e. the jelly comes out. This goo can then press on nerves and other tissues, causing a variety of symptoms besides pain and inflammation to occur.
Symptoms of a Herniated Disc
You can get a herniated disc between any vertebrae, from the cervical spine (neck) to the lumbar region (lower back). However, they most often occur in the lower back. Symptoms can vary depending on where the herniation occurred and the severity of the burst.
People who have a herniated disc may experience:
- Lower back pain
- Inflammation
- Numbness or tingling in your extremities (arms, legs, hands, feet)
- Muscle spasms
- Loss of bladder control
- Heavy feeling in your limbs
- Loss of coordination
- Weakness
- Difficulty walking
That said, while some patients can experience one or many of these symptoms, others feel nothing at all and don’t even know they have a herniated disc. The onset of symptoms depends on the severity of the rupture and which nerve it’s pressing on.
What Causes a Herniated Disc?
This ailment is most often caused by age. Over time, the discs lose water content, causing them to shrink and pinch nerve roots. Formally known as disc degeneration, this disease has similar symptoms as a burst disc. The fibrous collagen layer may also develop tiny microtears from this and eventually burst when it becomes too weak.
It might also not be the first time the disc burst. Because discs burst without revealing any symptoms, your disc could have ruptured and healed several times over before symptoms arise. The more it bursts, the weaker the protective wall gets.
Other causes may include:
- Twisting and turning while lifting
- Overstress, such as lifting heavy objects
- Stress fractures
- Spinal injuries
- Congenital abnormalities
Will a Herniated Disc Heal on Its Own?
Yes, most herniated discs heal on their own. Because the jelly is not where it’s supposed to be, the body treats it like a foreign object. The jelly will first be cleared by special cells called macrophages and monocytes, and then the collagen fibers will eventually heal back in the form of scar tissue. However, this scar tissue is weaker than the original fibers, making that disc more susceptible to future herniations.
Only in rare cases do herniated discs require surgery. However, this can vary person-to-person — and yes, even the self-healing ones can be very painful if not treated properly.
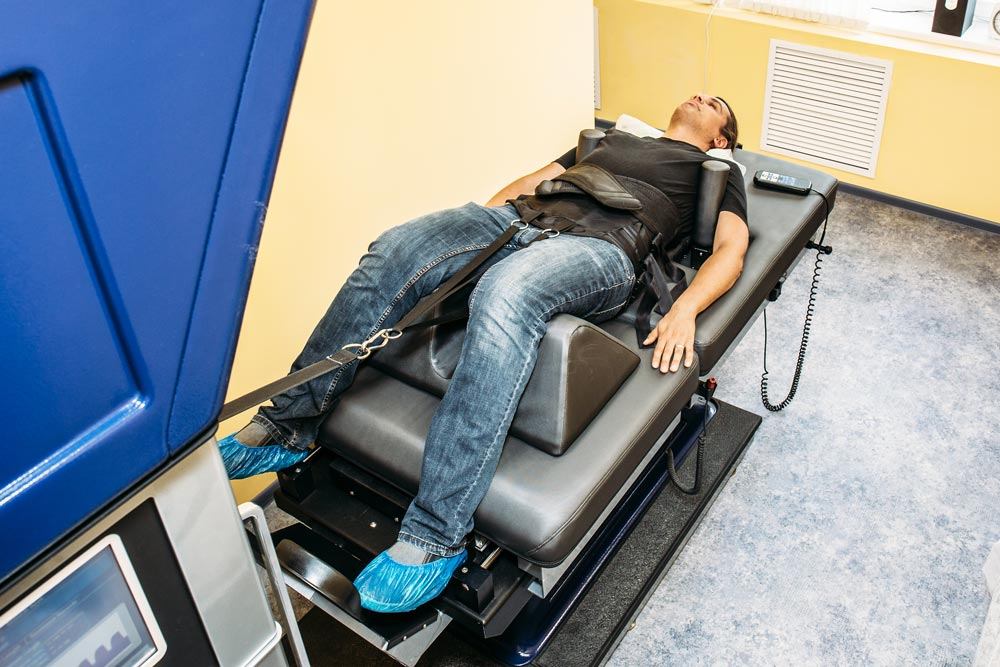
The DRX9000 spinal decompression machine can be an effective treatment for herniated discs.
Non-Surgical Treatment Options for Herniated Discs
You don’t have to bear the potential pain of a herniated disc as it heals. If you suspect you are experiencing pain caused by a herniated disc, contact Texas Spine clinic or your chiropractor. You need an accurate diagnosis for your pain, such as with a CT scan, an MRI, or an X-ray.
Thankfully, multiple treatment options can successfully deliver the long-term pain relief you’re seeking via non-invasive and minimally invasive solutions. Those include:
- Pain medication, such as NSAIDs to reduce inflammation and relieve pain
- Epidural steroid injections to reduce inflammation and control pain
- Lifestyle changes, such as exercise and dieting
- Physical therapy, such as back-strengthening exercises to correct your posture
- Cold and hot compresses to either reduce inflammation or relieve pain
- Radiofrequency ablation, which burns off the affected nerve
- Facet blocks to calm down an inflamed pinched nerve
Seek Medical Care for Your Pain
If you’re actively in pain, we always recommend you seek medical advice from a chiropractor or doctor. Without an accurate diagnosis and proper treatment, your symptoms may worsen over time.
Herniated discs also can and do cause extreme numbness, loss of touch sensations, and bowel dysfunction. Even worse, some conditions may require immediate care such as Cauda Equina Syndrome, a serious medical emergency that causes a loss of bowel or bladder control and numbness around the anus.
If you’re in the San Antonio area and are experiencing back pain, call Texas Spine Clinic today to schedule a risk-free appointment. You are in control of your pain!